Parotidectomy
This leaflet provides information about parotidectomy surgery, its purpose, what to expect before, during, and after the procedure, and potential risks and complications. It is designed to help you understand the procedure and make informed decisions about your care. Please do not hesitate to discuss any questions or concerns with me or my team.
What is the Parotid Gland?
The parotid glands are the largest of the salivary glands. You have two parotid glands, one on each side of your face, located just in front of your ears and extending down towards your jawline. These glands produce saliva, which plays a crucial role in:
- Digestion: Saliva helps break down food, making it easier to swallow.
- Oral Hygiene: Saliva washes away food particles and bacteria, protecting your teeth and gums.
- Lubrication: Saliva keeps your mouth moist, allowing for comfortable speaking and eating.
Why Might I Need a Parotidectomy?
A parotidectomy is the surgical removal of all or part of the parotid gland. It is typically recommended for the following conditions:
- Tumours: The most common reason for a parotidectomy is to remove a tumour in the parotid gland. These tumours can be benign (non-cancerous) or malignant (cancerous).
- Infections: Chronic or recurrent infections of the parotid gland that don't respond to other treatments may require surgical removal.
- Salivary Stones: Large or recurring salivary stones that block the flow of saliva can sometimes necessitate removal of the affected portion of the gland.
- Cysts: Fluid-filled sacs (cysts) within the parotid gland can sometimes require surgical excision.
What Happens Before Surgery?
Before your parotidectomy, I will conduct a thorough evaluation to assess your overall health and the specific characteristics of your condition. This may involve:
- Physical Examination: I will examine your parotid gland and surrounding areas.
- Imaging Studies: You may undergo imaging tests like a CT scan, MRI, or ultrasound to visualize the gland and any abnormalities.
- Fine Needle Aspiration (FNA): If a tumour is suspected, a small sample of cells may be collected using a fine needle for examination under a microscope. This helps determine if the tumour is benign or malignant.
- Medical History Review: I will review your medical history, including any medications you are taking, allergies, and previous surgeries. I will discuss the surgical procedure with you in detail, explaining the benefits, risks, and alternatives. I will also provide instructions on how to prepare for surgery, such as fasting and adjusting medications.
What Happens During Surgery?
A parotidectomy is performed under general anaesthesia, meaning you will be asleep throughout the procedure.
The Extent of Removal
The specific amount of the gland removed depends on the size and location of the problem:
- Extracapsular Dissection (ECD): This is a minimally invasive technique often used for small, benign, mobile lumps. Instead of dissecting the main trunk of the facial nerve, the tumour is removed with a small "cuff" of healthy tissue surrounding it. This preserves more of the gland and reduces the risk of the face looking hollow.
- Superficial Parotidectomy: This involves removing the superficial lobe of the parotid gland, which sits on top of the facial nerve. This is the standard operation for most parotid tumours. The facial nerve is carefully identified and preserved.
- Total Parotidectomy: This involves removing the entire parotid gland, including the superficial and deep lobes (the portion underneath the facial nerve). This procedure is typically reserved for malignant tumours or extensive benign tumours.
Surgical Approaches and Scars
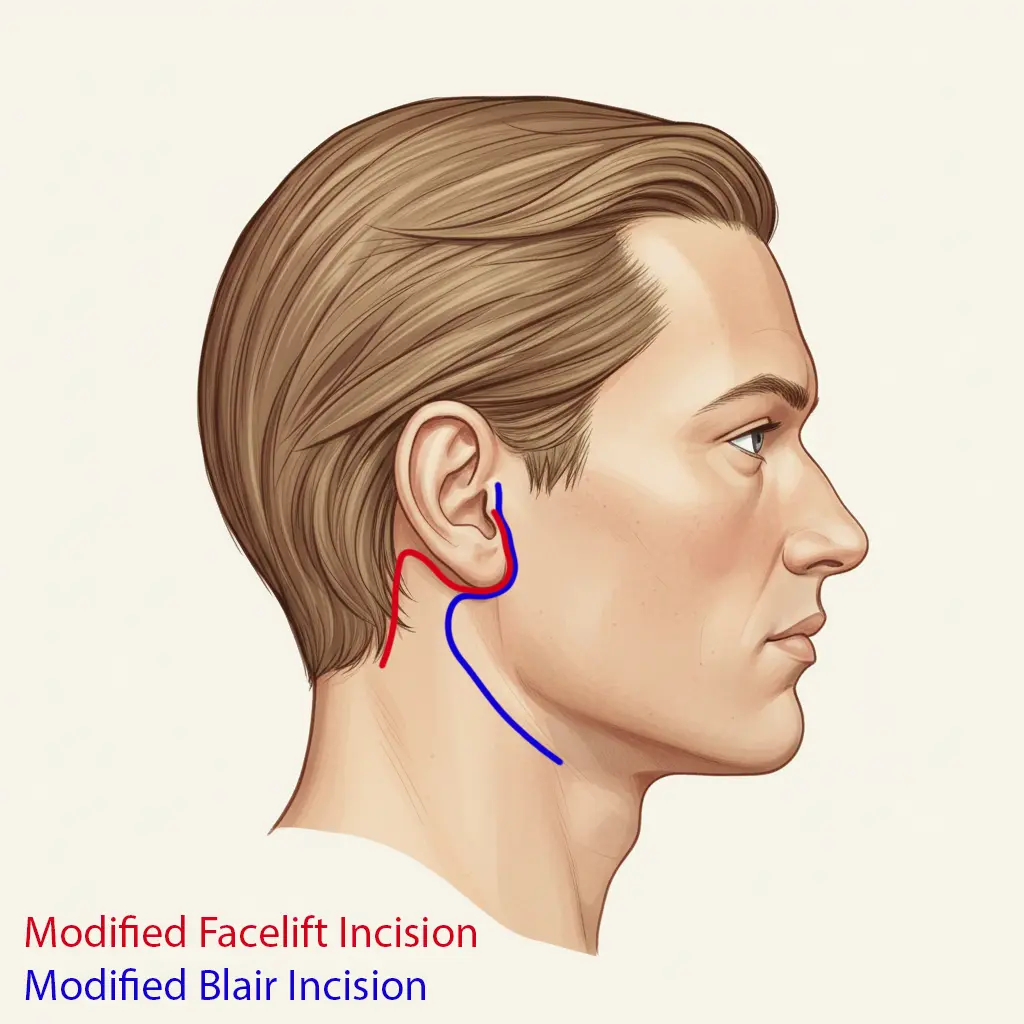
The type of incision (cut) used during your surgery depends on the location of the tumour and cosmetic considerations. We will discuss which approach is best for you:
- Modified Blair Incision (The Standard Approach): This is the safest and most common approach. The incision begins in the natural crease in front of your ear, curves around the earlobe, and extends down into a natural skin crease in the upper neck (in an "S" shape). This gives the best view of the facial nerve for safety. The scar usually heals very well and blends into natural neck creases.
- Facelift Incision: For suitable patients (usually those with small, benign tumours in the lower gland), we may use a cosmetic facelift approach. The incision is hidden inside or just in front of the ear canal, travels around the earlobe, and extends behind the ear into the hairline. This avoids a visible scar on the neck.
After removing the affected portion of the gland, the incision is closed with sutures. A small drain may be placed to remove excess fluid and blood.
What Happens After Surgery?
After surgery, you will be monitored in the recovery area until you are awake and stable. You can expect some pain and swelling in the area, which can be managed with pain medication. The drain, if placed, is usually removed within a few days. I will provide instructions on wound care, pain management, and activity restrictions. You may need to follow a soft food diet for a few days. It's important to avoid strenuous activity and protect the incision site from direct sunlight. Most patients can return home within a day or two after surgery. I will schedule follow-up appointments to monitor your recovery and discuss any further treatment, if necessary.
What are the Potential Risks and Complications?
While parotidectomy is generally a safe procedure, like any surgery, it carries potential risks and complications. These can include:
- Facial Nerve Weakness or Paralysis: The facial nerve runs through the parotid gland, and there is a risk of temporary or permanent weakness or paralysis of the facial muscles (causing a lopsided smile or inability to close the eye). Meticulous care is taken to identify and preserve the facial nerve during surgery, minimizing this risk.
- Frey's Syndrome: This condition, also known as gustatory sweating, can occur after parotidectomy. It causes sweating on the cheek or side of the face when eating.
- Numbness: You will likely experience numbness in the earlobe and the skin around the incision. This is due to the disruption of small sensory nerves and is often permanent, though it becomes less bothersome over time.
- Salivary Fistula or Sialocele: Occasionally, saliva may leak from the cut surface of the remaining gland. It can form a collection under the skin (sialocele) or leak through the wound (fistula). This usually resolves with conservative management.
- Infection: As with any surgery, there is a risk of infection at the incision site.
- Haematoma: A collection of blood can form under the skin, which may require drainage. These complications will be discussed with you in detail before surgery. I will also explain the steps taken to minimize these risks and how they would be managed if they were to occur.
Long-Term Outlook
The long-term outlook after parotidectomy is generally good. Most patients recover fully and experience no significant long-term complications. If a tumour was removed, the likelihood of recurrence depends on the type and stage of the tumour. I will discuss your individual prognosis with you after surgery.
Recovery and Returning to Normal Activities
Recovery time after parotidectomy varies depending on the extent of the surgery and individual healing. Most patients can resume normal activities within a few weeks. I will provide specific guidance on when you can return to work, exercise, and other activities.
Living with a Single Parotid Gland
If you have a total parotidectomy, you will be left with only one parotid gland. The remaining gland (and the other smaller salivary glands) is usually able to produce enough saliva to maintain adequate oral moisture. You may experience some dryness in your mouth, which can be managed with artificial saliva or frequent sips of water.
